This is a post about our latest publication in Blood reviews.
You can download our paper for free for the next 50 days from this link.
Platelets and inflammation
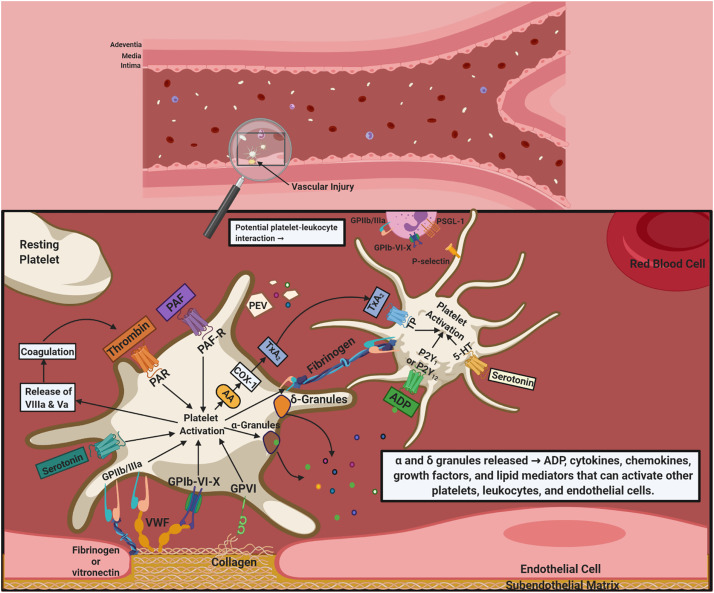
Platelets are central to inflammation-related manifestations of cardiovascular diseases (CVD) such as atherosclerosis. Platelet-activating factor (PAF), thrombin, thromboxane A2 (TxA2), and adenosine diphosphate (ADP) are some of the key agonists of platelet activation that are at the intersection between a plethora of inflammatory pathways that modulate pro-inflammatory and coagulation processes. The aim of this article is to review the role of platelets and the relationship between their structure, function, and the interactions of their constituents in systemic inflammation and atherosclerosis. Antiplatelet therapies are discussed with a view to primary prevention of CVD by the clinical reduction of platelet reactivity and inflammation. Current antiplatelet therapies are effective in reducing cardiovascular risk but increase bleeding risk. Novel therapeutic antiplatelet approaches beyond current pharmacological modalities that do not increase the risk of bleeding require further investigation. There is potential for specifically designed nutraceuticals that may become safer alternatives to pharmacological antiplatelet agents for the primary prevention of CVD but there is serious concern over their efficacy and regulation, which requires considerably more research.
Aim of the paper
While the chief role of platelets is to prevent blood loss in response to tissue injury, platelets are accountable for the formation of pathogenic thrombi that lead to manifestations of acute vascular atherothrombotic diseases [10]. Platelets are also mediators of inflammation and immunomodulatory activity that contributes to the development of atherosclerosis . The aim of this review is to provide an overview of platelet-associated pro-inflammatory and prothrombotic pathways and to discuss the potential role of antiplatelet therapy in preventing the onset and development of atherosclerosis.
Conclusions and future perspectives
The unique structure and biofunctionality of platelets is a major contributory factor for the successful completion of their haemostatic mechanisms, but is also influential in the pathology of chronic diseases. This review highlights that platelets and platelet-derived molecules, including prothrombotic mediators, are directly implicated in a plethora of complex mechanisms that initiate and propagate chronic manifestations related to inflammation and thrombosis, such as atherosclerosis and atherothrombosis. Antiplatelet therapeutic strategies for primordial prevention of CVD are almost non-existent, but there is potential for the development of novel nutraceuticals that may supplement or form part of the everyday diet. Antiplatelet therapies for the primary prevention of CVD are well-established for high-risk patients. However, further research is required to develop novel or complimentary antiplatelet treatments for the prevention of atherothrombosis and related cardiovascular events with lower risks to patients.